Placenta Previa 2013
-
Upload
rendy-adhitya-pratama -
Category
Documents
-
view
224 -
download
0
Transcript of Placenta Previa 2013
-
7/30/2019 Placenta Previa 2013
1/23
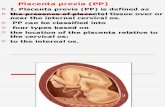
Placenta previa (PP)
I. Placenta previa (PP) is defined as
the presence of placental tissue over ornear the internal cervical os.
PP can be classified into
four types based on the location of the placenta relative to
the cervical os:
to the internal os.
-
7/30/2019 Placenta Previa 2013
2/23
-
7/30/2019 Placenta Previa 2013
3/23
-
7/30/2019 Placenta Previa 2013
4/23
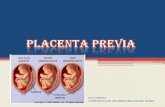
complete or total previa,
the placenta covers the entire
cervical os; partial previa,
the margin of the placenta coverspart but not all of the internal os;
marginal previa,
the edge of the placenta liesadjacent to the internal os;
low-lying placenta, placenta is located near (2 to 3 cm)
but not directly adjacent
-
7/30/2019 Placenta Previa 2013
5/23
A. Epidemiology
1. the incidence of PP is 1 in 200 to 1 in 390
pregnancies over 20 weeks' gestational age).varies with parity,
For nulliparous, the incidence is 0.2%,
in grand multiparous, it may be as high as 5%2. The most important risk factor for PP is aprevious cesarean section.
PP occurs in 1% of pregnancies after a
cesarean section.The incidence after four or more cs increasesto 10%
-
7/30/2019 Placenta Previa 2013
6/23
3. Other risk factors
increasing maternal age after age 40),
multiple gestation, and previousuterine curettage
4. the placenta covers the cervical os
in 5% of pregnancies when examinedat midpregnancy.
The majority resolve as the uterusgrows with gestational age.
The upper third of the cervix developsinto the lower uterine segment, and
the placenta "migrates" away from theinternal os.
-
7/30/2019 Placenta Previa 2013
7/23
B. Etiology. unknown.
a. Endometrial scarring.
b. A reduction inuteroplacental oxygenpromotes need for an increasein the placental surface areathat favors previa places.
-
7/30/2019 Placenta Previa 2013
8/23
2. Bleeding occur in association with
the development of the lower uterine
segment in the third trimester.
Placental attachment is disrupted
because this area gradually thins in
preparation for labor.
-
7/30/2019 Placenta Previa 2013
9/23
the thinned lower uterine segment is
unable to contract adequately to
prevent blood flow from the openvessels.shearing action
3. Vaginal examination or
intercourse may also cause separationof the placenta from the uterine wall.
-
7/30/2019 Placenta Previa 2013
10/23
C. Clinical Manifestations
1. 80% of affected patients presentwith painless vaginal bleeding
Most commonly,
the first episode is around 34 weeks ofgestation;
one-third of patients develop bleedingbefore 30 weeks
-
7/30/2019 Placenta Previa 2013
11/23
2. 30% patients develop bleedingafter 36 weeks,
10% go to term without any bleeding
The fluid is usually bright red,
and the bleeding is acute in onset.
3. The number of bleeding episodes is
unrelated to the degree of placentaprevia or
the prognosis for fetal survival.
-
7/30/2019 Placenta Previa 2013
12/23
4. pp is associated with a doubling ofthe rate of congenital malformations.
a. CNS, GI tract, cardiovascularsystem, and respiratory system
b. Pp is also associated with
fetal malpresentation, preterm premature rupture of
membranes, and
intrauterine growth restriction.
-
7/30/2019 Placenta Previa 2013
13/23
c. Abnormal growth of the placentainto the uterus can result in one of thefollowing 3 complications:
i. Placenta Previa Accreta.
The placenta adheres to the uterinewall without the usual interveningdecidua basalis.
The incidence in patients with previawho have not had previous uterine
surgery is 4%. The risk is increased 25%
in patients who have had a previous
cs or uterine surgery
-
7/30/2019 Placenta Previa 2013
14/23
ii. Placenta Previa Increta.
placenta invades myometrium.
iii. Placenta Previa Percreta.
The placenta penetrates the
entire uterine wallgrowing into bladder or bowel.
-
7/30/2019 Placenta Previa 2013
15/23
D. Diagnosis
1. History.
PP presents with acute onset ofpainless vaginal bleeding.
A thorough history should be obtained
from the patient, including obstetricand surgical history as well asdocumentation of previous ultrasoundexaminations.
Other causes of vaginal bleeding mustalso be ruled out, such as placentalabruption.
-
7/30/2019 Placenta Previa 2013
16/23
2. Vaginal sonography is the goldstandard for diagnosis of previa
Placental tissue has to be overlying orwithin 2 cm of the internal cervical os tomake the diagnosis.
The diagnosis may be missed bytransabdominal scan,
if the placenta lies in the posteriorportion
empty bladder may help in identifyinganterior previas, and
Trendelenburg positioning may be
useful in diagnosing posterior previas.
-
7/30/2019 Placenta Previa 2013
17/23
-
7/30/2019 Placenta Previa 2013
18/23
3. Examination. IfPP is present, digitalexamination is contraindicated.
a. A speculum examination can beused to evaluate the
b. Maternal vital signs,
abdominal exam, uterine tone, and
fetal heart rate monitoring should beevaluated.
-
7/30/2019 Placenta Previa 2013
19/23
E. Management
1. Standard Management
a. In the third trimester in a patient whois not bleeding,
recommendations include
ultrasound confirmation
pelvic rest (nothing in the vagina,including intercourse or pelvic exams),
explanation of warning signs and when toseek immediate medical attention,
avoidance of exercise and strenuousactivity,
and fetal growth ultrasounds every 3 to 4weeks.
Fetal testing semiweekly
b S d d f
-
7/30/2019 Placenta Previa 2013
20/23
b. Standard management ofsymptomatic patients with PP
hos-pitalization with hemodynamic
stabilization and
continuous maternal and fetalmonitoring.
Laboratory studies should be ordered Steroids should be given to promote
lung maturity for gestations between
24 and 34 weeks. Rho(D) immunoglobulin should be
administered to Rh-neg-ativemothers.
-
7/30/2019 Placenta Previa 2013
21/23
2. Term Gestation, Maternal andFetal Hemodynamic Stability.
At this point, management dependson placental location.
a. Complete Previa.
Patients with complete previa atterm require cesarean section.
-
7/30/2019 Placenta Previa 2013
22/23
-
7/30/2019 Placenta Previa 2013
23/23
3. Term Gestation,
Maternal and Fetal
Hemodynamic Instability. The first priority is to stabilizethe mother with
fluid resuscitation and administration of bloodproducts, if necessary.